[ad_1]
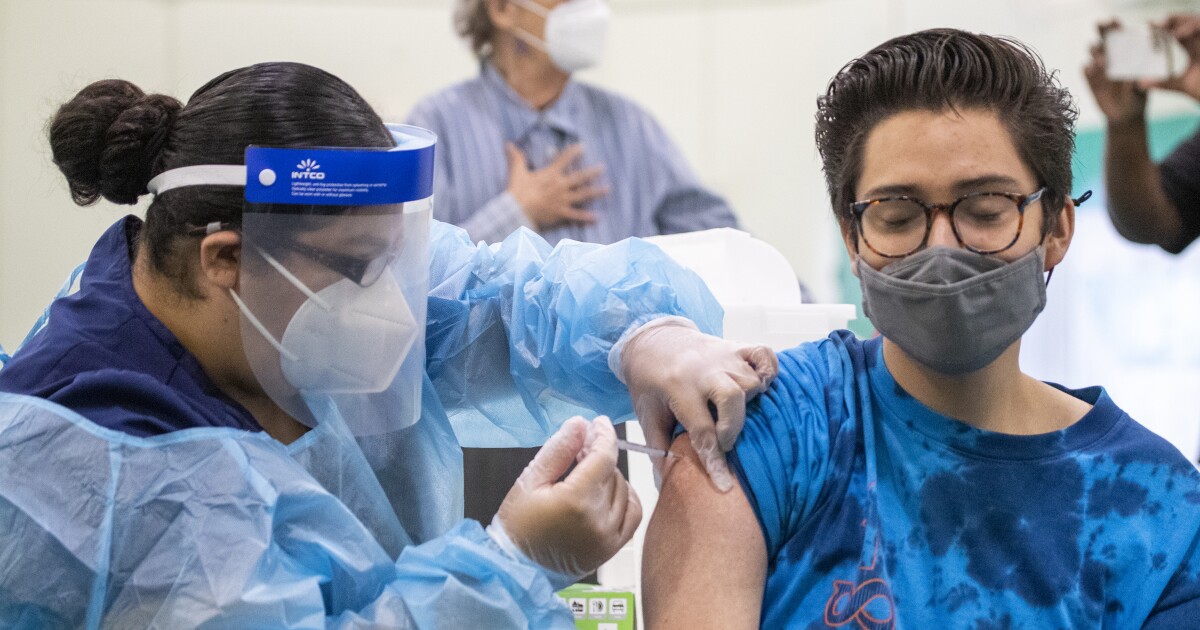
Booster shots are allowed for all American adults, but some wonder if they need them. A nurse fills a syringe with Pfizer-BioNTech Covid-19 at an pop-up vaccination clinic in the Arleta neighborhood of Los Angeles, California.
ROBYN BECK / AFP via Getty Images
hide caption
toggle legend
ROBYN BECK / AFP via Getty Images

Booster shots are allowed for all American adults, but some wonder if they need them. A nurse fills a syringe with Pfizer-BioNTech Covid-19 at an pop-up vaccination clinic in the Arleta neighborhood of Los Angeles, California.
ROBYN BECK / AFP via Getty Images
Federal health officials are urging Americans to boost their immunity before the winter break by getting vaccinated against COVID-19. But not everyone works with the same defenses when it comes to keeping the virus at bay.
More than 47 million people in the United States have already contracted the coronavirus, at least according to officially recorded figures. In reality, it’s probably several million more.
An unknown portion of these people are also vaccinated, which means they now have what scientists call hybrid immunity. This is what happens when your immune system has essentially done both a dress rehearsal to fend off the virus – thanks to the vaccine – and a real live performance – thanks to the virus.
So if you’ve ever had a symptomatic case of COVID, do you really need a booster?
It’s probably no shock that scientists are still not quite sure. Boosters have not been available for that long to most Americans, and studies to understand how necessary they are for everyone – let alone those who have been infected and vaccinated – have yet to be done.

But scientists say their best guess is that, by all accounts, people with hybrid immunity already have better immunity than vaccinated people who have never received COVID or people who have received COVID but not. the vaccine.
“It’s fair to say that your immunity is probably going to be stronger, so the risk of getting sick, especially with the delta variant, is very, very low,” says Dr Duane Wesemann, immunologist at Brigham and Women’s Hospital and Harvard Medical School.
Think of the immune system and the coronavirus as if you were learning an instrument: train once and you’ll remember the song the next day, but – if you stop – you probably won’t do it a year later. “The same principles apply to the immune system,” explains Wesemann. “You will spend more time, invest more effort in holding onto something that you have seen many times.”
And if you’ve been infected and vaccinated, that’s already a lot of practice.
Just because you have this more robust immunity doesn’t mean it’s a bad idea to get a booster, though. This is especially true if you’re already predisposed to developing severe COVID-19, says John Wherry, director of the Institute of Immunology, University of Pennsylvania.
It’s all still under investigation, but Wherry says there’s no reason to think it would be risky for people with hybrid immunity to receive an additional injection.
“The safety profile looks quite similar during the primary series and boosters and it doesn’t look very different depending on whether or not you’ve had COVID before,” he says.
Our best picture of the powers of hybrid immunity comes from studying people infected and then vaccinated – what some scientists have even described as “superhuman immunity.”
“Looks like you’re already getting a callback in a pretty spectacular way,” says Wherry. “They would probably be the lowest on my priority list of those in need of a booster.”
Research shows that people with this type of hybrid immunity produce more antibodies and this response is not only more stable, but is really robust across variants, says Wesemann, whose lab has studied the immune response in people who are subsequently infected and vaccinated.
So what about a person’s level of protection for the reverse scenario – when a fully vaccinated person later has a breakthrough infection? “You would probably have superior immunity at this point,” says Dr Gregory Poland, director of the Mayo Clinic’s vaccine research group.
Most likely, this brand of hybrid immunity would rival what is seen in people who have recovered from COVID-19 and then got vaccinated, but there could be subtle differences in the details of the immune response, Wherry said. “But those things that might be different may not matter for a particular person to avoid the next infection.”
All of this must be studied to arrive at a more conclusive answer. Until then, the take-out is the same no matter how you came up with hybrid immunity: there is no great rush to get a booster for people who are otherwise healthy. and low risk. But if you are at a higher risk due to underlying conditions, or if you live or work closely with someone who is, it could be a good extra layer of protection, for you and those around you.
“The potential benefits of providing greater immunity are there and the risks are low,” explains Wesemann. “I would probably recommend it to a group of people who I thought were at high risk.”
[ad_2]
Source Link